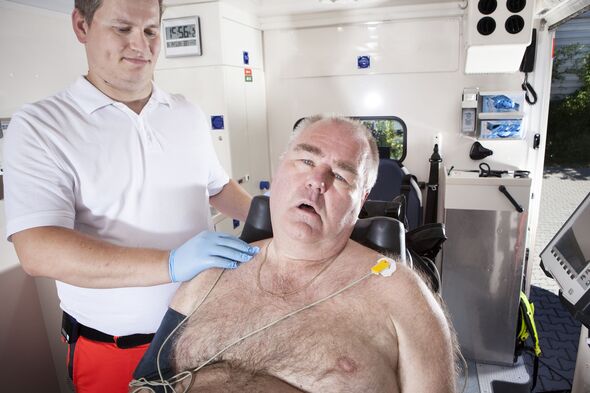
The National Health Service (NHS) has reported a significant increase in spending on services related to obesity, with expenditures on specialist ambulances and equipment surpassing £20.7 million since 2020. This rise, revealed through data obtained under Freedom of Information laws, underscores the escalating demand for tailored healthcare solutions for patients with obesity and severe mobility challenges.
In 2024 alone, NHS ambulance trusts across the United Kingdom collectively spent £4.98 million on bariatric ambulances, marking the highest annual figure in a five-year span. The data indicates a staggering increase of 123 percent in spending between 2023 and 2024, reflecting the urgent need for vehicles and equipment designed to accommodate heavier patients.
According to research commissioned by the online pharmacy Chemist4U, there have been at least 157,240 emergency call-outs requiring a bariatric ambulance or associated equipment since 2020. This figure is likely an underrepresentation, as some ambulance trusts utilize bariatric-equipped vehicles for all emergency responses.
Rising Costs and Health Implications
A spokesperson for West Midlands Ambulance Service stated, “Like all ambulance trusts, West Midlands Ambulance Service has a specialist bariatric capability for those patients that require it. All of our emergency ambulances are bariatric capable, but in addition, we have vehicles fitted with specialist stretchers and lifting and handling kit over and above that carried on our standard fleet.”
Government estimates predict that the financial burden of obesity on the NHS will reach £11.4 billion by 2025, nearly doubling from the £6.5 billion projected in 2023. Obesity is linked to various health issues, including cardiovascular disease, type 2 diabetes, strokes, and certain cancers. Public Health England has reported that two-thirds of adults in England are classified as overweight or obese, and concerning trends are emerging among children as well.
In 2023, one in five children starting primary school was either overweight or obese, escalating to one in three by Year 6. These figures have remained high since the COVID-19 pandemic, with disadvantaged areas experiencing the most pronounced increases. A 2024 report from NHS England warned that the rising obesity rates among children could lead to unprecedented numbers of teenagers requiring treatment for type 2 diabetes and musculoskeletal disorders within the next decade.
Challenges Ahead for the NHS
Jason Murphy, Head of Pharmacy at Chemist4U, commented on the implications of the new data. He emphasized that the increase in expenditure on bariatric ambulances and equipment showcases the profound impact of obesity and related health challenges across the UK. “Reducing the number of obese individuals will not only alleviate spending on specialist equipment but also decrease the treatment costs associated with diseases linked to obesity, including heart disease, diabetes, and some cancers,” Murphy stated.
The NHS faces substantial challenges as it grapples with a growing patient population requiring specialized care. The financial implications of obesity continue to rise, prompting urgent discussions on public health initiatives aimed at reducing obesity rates and improving overall health outcomes. As the crisis deepens, the health service’s capacity to address these issues will be critical in managing future demands.